
Three-year-old Lana toddles around the living room in the Grinberg family’s Plymouth home. What’s immediately remarkable about Lana is that she’s bilingual, with her dad speaking to her only in Russian. But hearing Lana’s story from her parents, Gaby Israel Grinberg and Mike Grinberg, it’s clear that Lana is remarkable in many ways, as are her parents.

Lana, Gaby and Mike, the Grinberg family
Born at 24 weeks gestation and weighing 330 grams (about 11 ounces) at birth, Lana is the second smallest baby to be born and survive at Children’s Minneapolis hospital. Lana was due to arrive in December 2015. In August, Gaby began experiencing symptoms of pre-eclampsia and HELLP syndrome but, unfortunately, she was not correctly diagnosed at the time. Preeclampsia is a condition affecting at least 5-8 percent of all pregnancies. It causes high blood pressure, protein in the urine and swelling. It usually occurs in the 20th week of pregnancy but can appear sooner or later. If preeclampsia progresses to eclampsia, seizures and even death can occur. HELLP syndrome stands for hemolysis (the breaking down of red blood cells), elevated liver enzymes and low platelet count.
Gaby’s first trimester was uneventful. At 31, her pregnancy was not considered high-risk. She experienced extreme morning sickness, but thought that it was a normal part of pregnancy. “At my 20-week ultrasound, the doctors realized something was wrong,” Gaby says. “The OB said that my amniotic fluid was low, and that Lana was about two weeks small for her gestational age,” says Gaby.
“My regular OB did not have an explanation for why this was happening and told me that I was now considered high-risk and would need to transfer my care to a perinatal clinic,” says Gaby. “I was told it could be anything from an infection in utero, to Down syndrome to something congenital.”
At their first appointment at the perinatal clinic, a level 2 ultrasound was done, which confirmed what they were told earlier—low amniotic fluid and small measurements for the baby.
“We were able to rule out many genetic diseases and issues … Lana was ‘healthy’ and anatomically correct and all there, but there was still no explanation of what was happening and why,” says Gaby.
Gaby was advised to resume normal activity and to call her regular OB with any concerns. She was told to return in three weeks, which would have been her 24th week of pregnancy.

Lana’s diapers from birth through her first year.
Gaby says that about a week later, she started to feel increased nausea, abdominal pain, and other symptoms. She called her regular OB doctor twice, and was told her symptoms were due to round ligament pain. This was “despite the other symptoms and … the fact that I reminded them I was high risk,” says Gaby. “I was misdiagnosed.”
“Later that week because I really had not been feeling well … Mike insisted we go to the Mother Baby Center for a maternal/fetal check-up. According to them, I was fine, baby was fine.” She was told there were no issues, and to call or come back if her situation changed, she says.
A few days after that, Gaby’s symptoms peaked. “I was short of breath and had severe chest pain and tightness,” she says. “It was so bad, I thought I was having a heart attack.” Mike took Gaby to the Mother Baby Center where she underwent an ultrasound and fetal monitoring. “We were told that everything looked okay, but to come back if anything changed.”
The Grinbergs returned home, but Gaby’s chest pain became even more severe, and they returned to the center, where she was immediately admitted. “A perinatal surgeon and the OB who saw me initially told me that I might have preeclampsia and HELLP syndrome.”
Gaby could tell by looking at her husband’s face that something was very seriously wrong. “Mike usually looks calm in any circumstance, but I could see the fear and stress.” Gaby was hooked up to IVs.
Gaby was told that her blood pressure was 190/120, and “I was very dangerously close to having a stroke, and that depending on whether they were able to stabilize my condition, and they were very careful not to say preeclampsia or HELLP Syndrome just yet, that I may have to deliver my baby,” says Gaby.
“I was shocked at being told my life was at risk,” she says.
Gaby was treated with large doses of magnesium, intravenous fluids and steroids to help the baby’s lungs develop. “We were put into the antepartum wing. Their purpose is to do everything they can to keep the baby inside. They have to balance what’s best for the mother with what’s best for the baby,” Gaby says. “The nurses there were like angels.”
After a week in the Mother Baby Center, Gaby’s symptoms worsened. “We were told, ‘We’re going to have to do it,’ meaning that they were going to have to deliver the baby,” because at this point, both Gaby’s life and the baby’s were in jeopardy. So at 24 weeks gestation, Gaby underwent an emergency C-section.
Mike says, “We were told that the odds for survival and a normal life were very low, and that Lana could have brain damage or cerebral palsy. We told the doctors that we wanted the best possible chance for her.”
Gaby adds, “We wanted to give Lana the best quality of life for as long as possible.”
The Grinbergs have high praise for Dr. Jeanne Mrozek, head neonatal physician for the Minnesota Neonatal Physicians Group, who was one of several physicians doing rounds at Children’s. “We are so lucky we got the care we did from Dr. Mrozek and other doctors,” says Gaby.
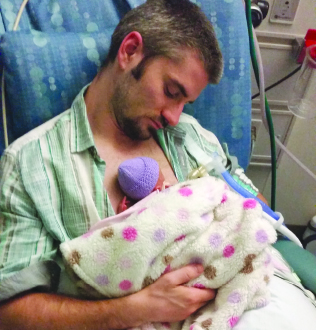
Mike holding Lana in the hospital

Mike holding some of her early hat and booties (knitted by friends and family)
Lana spent six long months in the NICU. Part of Lana’s hospital stay included surgery to close the valve from her heart to her lungs, which is normally open in utero, but closes close to the time of a full-term birth, says Gaby.
What were the factors that helped Lana survive and thrive? Mrozek says, “Children’s has a history of being very proactive about giving patients a chance.” She explains that some hospitals are not as proactive because of the high risk for challenging outcomes. “There are concerns about cerebral palsy and cognitive delays. But we know that kids can have those diagnoses and live full and meaningful lives in the face of challenging situations,” she says.
“Lana was blessed with great parents,” says Dr. Mrozek. “They were very involved and were strong advocates for her care.” She explains that skin-to-skin contact, known as “kangaroo care” is very important for a good outcome. “Both of Lana’s parents were very vigilant about giving Lana as much skin-to-skin contact as possible while Lana was in the NICU. It improves short-term and long-term outcomes. It literally helps with brain development. And we have a very broad and dedicated team of nurses and physicians and team members—respiratory therapists, social workers, occupational therapists, developmental specialists. And she [Lana] is the reason we do it.”
Mrozek says that the team values the relationships they build with families and love to see the children’s progress. Families often send photos to the team as the children grow and develop.
As joyous as Lana’s release from the hospital was, returning home had its own challenges. Because of the months she had been on a ventilator, she was dependent on a feeding tube. This caused difficulty with oral feeding, so Lana had a feeding tube when she returned home, as well as supplemental oxygen.
While having a baby in the NICU is isolating, returning home was also isolating for Gaby. “I couldn’t even take her out in public because it was RSV (respiratory syncytial virus) season.
Gaby became a full-time caregiver, and the role was an extremely demanding one. Feeding remained difficult for Lana. Gaby had to keep track of Lana’s multiple appointments and frequently bring her to different specialists. The constant demands of caregiving combined with sleep deprivation took their toll. Gaby had severe anxiety, imagining scenarios of what could go wrong. She suffered from severe postpartum depression and developed PTSD (post-traumatic stress disorder.)
Gaby says that while they had a great deal of support from family and friends, her needs as a mom were not usually considered. “Everyone always asked, ‘How’s Lana?’ Seldom did anyone ask how I was doing.”
When Gaby began to think about ending her life, she realized she needed help. She began seeing a therapist.
A group called Twin Cities Mameles was invaluable to the Grinbergs. “We had meals prepared for us by people from friends to complete strangers. I don’t think we could have gotten through it without them.”
Shortly after Lana was born, Gaby had lost her job because of the time she had to take off from work for health needs, she says.
“While it was a devastating blow … it was in many ways a blessing in disguise as I required about eigtht to ten weeks of recovery after the C-section, and I was in no way mentally or emotionally prepared to go back to work,” she says.
“Overnight, I went from being a 30-something working professional soon-to-be mom, to a stay-at-hospital mom with my very premature baby girl, and what turned out to be a very long hospital stay.”
The Grinbergs turned their job situation into an opportunity—they started their own marketing business, Proofpoint Marketing, so that they could have control of their schedules and give Lana the attention she needed.
Giving back is important to the Grinbergs. They support Ronald McDonald House, which they say was invaluable to them during Lana’s hospitalization, as well as the March of Dimes and Preeclampsia Foundation.
Dr. Mrozek is also committed to to helping parents and caregivers of babies in the NICU. To this end, she founded and heads Minnesota Neonatal Foundation.
Grinbergs are working with Dr. Mrozek to find a meaningful way to be involved with the foundaiton.
“Long-term stays in the NICU are very hard for parents as well as for the caregivers,” Dr. Mrozek says. “I started the foundation for the express purpose of addressing the non-medical, psychosocial aspects. It can be socially isolating, even within families, since often it’s only the parents that fully understand the level of stress. … A lot of parents have PTSD, whether it’s diagnosed or not, and a lot of marriages don’t survive. People can’t do it alone.”
In June 2018, the foundation hosted their first NICU family reunion. Over 400 people attended, and some of the NICU graduates are now in their teens. The foundation also plans to hold wellbeing workshops, to help teach staff about grief, the importance of supporting each other and more. “If I can support the nursing staff, they will be better able to support families in crisis,” says Mrozek.
Mrozek’s advice for parents dealing with prematurity: “Have hope. These little babies have an amazing capacity for growth and limitless development. They change lives, even if they didn’t survive,” she says. “There’s an intangible that happens when you go through the fire and you come through the other side. I’m a great believer in the saying you don’t bounce back, you bounce through.”
More Info:
Minnesota Neonatal Foundation
www.neonatalfoundation.org
Preeclampsia Foundation
www.preeclampsia.org
Photos by Rachel Nadeau






















